Infusion Set & Sensor Problems? 15 Solutions to Reduce Irritation & Keep 'Em Stuck On
Michelle MacPhee
(D-Mom; Writer & Creator of WaltzingTheDragon.ca)
Here we share with you a comprehensive and objective review of number of different expert- and user-approved strategies to reduce the pain, hassle and obstacles of using insulin pumps and Continuous/Flash Glucose Monitoring systems... so you can keep using your insulin pump, CGM, or Libre!
SHARE THIS ARTICLE
Diabetes technologies like insulin pumps and glucose monitoring systems are life-changers. But for some, the use of these devices comes with adverse reactions to their infusion sets and sensors. At best these reactions impact the functioning of the device; at worst, they create pain, exasperation and health risks, compounding the burden of daily diabetes care. If you fall in this category, there’s hope! Even if you have already tried some basic skin prep products without success.
Our Family's Experience
My son has been using diabetes-tech for nine of the 11 years that our family has lived with type 1 diabetes. He got his first insulin pump a week after he turned three, and his first CGM a year later. Both brought new freedom and key information, changing how we managed diabetes within our family: he could have seconds, thirds and fourths without another shot; his blood glucose swings evened out because we could tailor insulin doses to his teeny body; we now had details about what was happening between finger pokes; we could see the effect certain foods had on his blood sugar; and we had warnings about lows (which he was otherwise unable to recognize at the time). Those were the golden years.
Skip ahead some years and we saw red, raised skin more often at the infusion site or sensor site. CGM readings started to get wonky; our trust in their accuracy was eroding. We were receiving wildly swinging glucose readings that did not match his symptoms, nor the fingerstick readings. Too often, the CGM was offline, producing only a series of question marks instead of glucose readings.
Once on a road trip home from a family gathering, the itching became so intense at the site that we had to remove his CGM sensor on the side of the highway. Then when we tried new technology a few years ago (Flash Glucose Monitoring) after a few days we discovered liquid seeping from the middle of the sensor housing. We took it off to find the skin underneath inflamed, painful and raw! In the exact shape of the sensor tape/housing, the skin had blistered and then the blisters had popped, leaving the tender skin exposed and extremely painful. It took several weeks to heal, and broke my heart to see my son suffering like that.
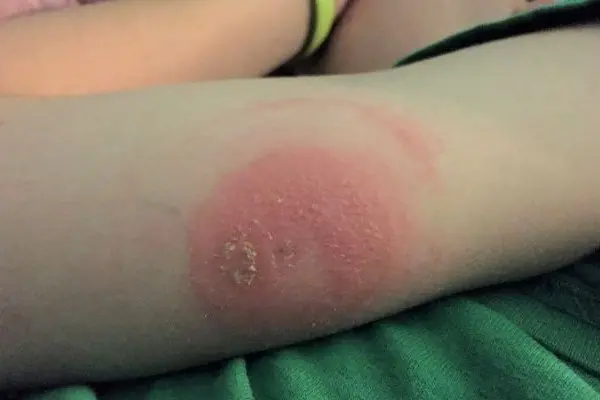
In an effort to find a device that would give us valuable blood glucose data while reducing the hassles of frequent finger pokes, we tried another manufacturer, just to find a similar reaction to those CGM sensors: a mushroom-shaped patch of inflamed and itchy skin was all the evidence we needed to convince us to press pause on glucose monitoring technology.
But now we've arrived at the right product and the right pre-insertion process to make it possible for our son to wear CGM again. (Yay!) And what we've found out along the way may help many of you overcome your own family’s struggles with infusion sets and/or sensors.
15 Steps to Reduce Skin Irritation, Itching and Pain… AND Keep Sets/Sensors On
A successful strategy to reduce or eliminate site irritation often depends upon the cause of the problem. Once you and your child’s health care team* have narrowed down the potential cause(s) of the trouble, there are a number of possible interventions which you can try in order to deal with the obstacles that get in the way of effective use of an insulin pump, CGM, or Flash glucose monitor.
(*To deal with skin reactions, your child's diabetes team may include your child’s endocrinologist, diabetes nurse, CDE (Certified Diabetes Educator), dermatologist, allergy specialist, or immunologist, or other health care professionals.)
Below are some potential solutions for you to consider, suggested by both experts in the diabetes field, as well as real-life d-tech users. You can pick and choose a few steps that are relevant to your individual issue, or you can go whole hog (if you do, it’s best to sequence them in the order presented). I would suggest trying new products alone first, to see if they’re tolerated well; if you’re using four applications and have a reaction to one, it will seem as if the whole process failed, when it might actually work if you used only the three products which do not lead to irritation.
Tips from the Trenches
You don’t have to trial the products with an actual infusion set or sensor. When we were trialing different products for future use, we would put a strip of Tegaderm, for example, on one part of our son’s body without a sensor, before using it with a functioning sensor. That way, if there was a reaction to the Tegaderm alone (and there was), we could simply remove it, lesson learned, without having wasted a sensor in the process. ~Michelle
Step 1. Try a Different Set or Sensor
The components that create problems in one product may be absent in another product. For this reason, a good first step may be to try products made by a different manufacturer.
Tips from the Trenches
When our son first started pumping, his skin reacted to the infusion sets that were distributed with his Animas pump. On a tip from another d-mom (WTD Co-Founder Danielle) we tried Accu-Chek® Ultraflex infusion sets, and the problem immediately went away. ~Michelle
Step 2. Let the Sensor Breathe
User-approved
Some community members have commented on the strong odor of plastic that they smell when they first open a sensor package (particularly Libre Flash Glucose sensors). These users suggest that after you open the sensor packaging, you let the sensor “air out” until it no longer smells like plastic before inserting it. They also suggest that they have found success with using a hair dryer to speed up this process.
Step 3. Numb the Site
Although numbing the site does not directly reduce skin reactions, if you use topical numbing as a pain reduction strategy, this is the place in the process in which you would use it.
Topical anesthetics have a numbing effect, so are used to block pain.
Some suggestions include:
- Apply ice directly to the skin at the infusion/sensor site by placing it in a thin facecloth or a plastic Ziploc bag, and then holding it against the skin for several seconds. (Expert- and User-approved)
- Gebauer's Pain Ease® is a “non-drug topical anesthetic skin refrigerant (vapocoolant) that begins working in just 4-10 seconds (to) temporarily control the pain associated with needle procedures (including immunizations, IV starts, blood draws). Intended for topical application on intact skin (and) minor open wounds.” (source: Gebauer.com) (Expert- and User-approved)
- GiGi topical Anaesthetic Numbing Spray: “within minutes… temporarily numbs the surface of the skin with a special Lidocaine based gel formula for sensitive skin”. (source: sallybeauty.com) (User-approved)
- EMLA™ topical numbing cream, which contains 2 numbing agents, lidocaine and prilocaine (2.5% each). (Expert-approved)
- Maxilene® topical numbing cream which contains Lidocaine as the numbing agent, available in either 4% or 5% strengths. (Expert-approved)
The creams need to be left on the skin for a period of time in order to take effect; a barrier tape such as Tegaderm or Opsite™ Flexifix™ over a dollop of cream will keep it in place for the required amount of time. The cream is then wiped off before moving on to the next step. (See manufacturer instructions for correct use of a particular product.)
Tips from the Trenches
Our family uses Maxilene®5 with 5% lidocaine because it’s stronger, and therefore has a quicker numbing effect, usually within 15 minutes. ~Michelle
More on Numbing:
Step 4. Cleanse the Site
Expert-approved
It’s important to thoroughly clean the skin in the area where you plan to insert the infusion set or sensor, both to reduce the bacteria on the skin that may cause an infection if it gets under the skin, as well as to remove any products that may cause irritation or keep the set from staying stuck on to the skin.
A variety of soaps or antiseptics cleansers can be used to cleanse the site. Some suggestions include:
- Dial® soap
- Hibiclens® antiseptic skin cleanser is “antimicrobial (kills or stops the growth of microorganisms), antiseptic (inhibits the growth of disease-causing microorganisms) and bactericidal (causes the death of bacteria) but gentle enough for routine family hand washing. Hibiclens begins killing germs on contact and continues killing up to 99% of germs for up to 24 hours.” (source: hibiclens.com)
- Betadine (Povidone-Iodine) wipes: Betadine is a “topical antiseptic that provides infection protection against a variety of germs for minor cuts, scrapes, and burns.” (source: betadine.com)
- BZK Antiseptic Towelettes contain Benzalkonium Chloride “for effective cleansing of wounds and skin. (They are) alcohol-free (and) do not sting.” (source: canadiansafetysupplies.com)
- IV-Prep™ (from Smith&Nephew) antiseptic wipes designed to sterilize and prepare skin prior to a ventipuncture or injection
- Alcohol swabs wipes (which often comes packaged with CGM/Flash sensors)
Tips from the Trenches
We found that using alcohol as a cleanser dried out our son’s skin too much, and actually caused more irritation than going without. We have found the most success with a mild soap. ~Michelle
In choosing a soap/cleanser, it may be helpful to keep in mind that perfumes/dyes may irritate the skin and so are best avoided. Also, if you have trouble with infusion sets/sensors falling off, it’s best to avoid Dove and other moisturizing soaps, as they interfere with adhesion. It’s such a balance between too dry and too moisturized!
More on Cleansing:
Step 5. Let the Skin Dry Completely
Expert-approved
Moisture trapped against the skin (under an adhesive product) can lead to irritation, regardless of whether you use any additional preps and products. For this reason, it’s important to allow the area to dry thoroughly and naturally between each step of preparation - without blowing on it, which can introduce bacteria to the area. This step is so critical, that if you are experiencing minor skin irritation, simply letting the area dry completely may resolve the problem, eliminating the need for further interventions.
Step 6. Apply an Anti-inflammatory Spray
Examples include:
- Anti-histamine Spray, such as Benadryl® topical Analgesic and Skin Protectant, which has as its medicinal ingredients: diphenhydramine hydrochloride (anti-histamine) and zinc acetate (astringent) to “relieve skin itch and pain: poison ivy, insect bites, allergic itch.” (Expert-approved)
- Steroid Asthma Spray, such as Flovent® (available by prescription only) or a steroid allergy spray, such as Flonase® Allergy Relief Aqueous Nasal Spray (available over the counter in Canada). These products contain fluticasone propionate as the medicinal ingredient (a corticosteroid), the original intention of which is to be sprayed into the nostrils to reduce allergy or asthma symptoms. However, when used to reduce sensor and infusion set inflammation, the product is sprayed right on the skin at the proposed site. (User-approved; also approved by some experts)
Although these products are only rated for up to 24-hour effectiveness in reducing itching and other inflammatory responses, it seems that when they effectively suppress the initial reaction at the time of insertion, that effect often lasts for the duration on the infusion set (2-3 days) or sensor (up to 7, or even 14 days); that is, if the initial reaction is interrupted, that may eliminate the reaction all together.
BUT… an important warning: corticosteroids (Flovent® and Flonase®) must be used with caution! We do not know the long term effects of consistent use of topical steroids, and those effects (which are likely to include the thinning of the skin, as well as permanent discolouration of the skin, among other undesired effects) could be more detrimental than the original reaction that we are trying to prevent. Therefore, it’s wise not to take the risk unless other, safer interventions have failed, and even then, only if your health care team agrees that the anticipated benefits outweigh the possible risks.
It’s important to note that the package insert for Flonase® allergy spray says it’s not recommended for children or adolescents under 18 unless on the advice of a doctor, if you are pregnant or breast-feeding, as well as a whole host of other exclusions (including an allergy to the contents of the spray); check with your health care team before use.
Step 7. Use a Liquid Barrier Wipe or Spray (to Decrease Irritation)
Expert- and User-approved
One way to protect the skin from the irritants that may be in the infusion set/sensor adhesive or plastic housing is to apply a layer of liquid, and then allow that liquid to dry into a film that acts as a barrier between the skin and the products that are applied over it.
Note that although 1-2 layers is usually enough, some users report needing up to 5 layers (letting each layer dry completely before applying the next layer) before the rash is successfully prevented.
Consider any one of the following barrier wipe trade names (in random order):
- Skin-Prep™ is a ”no-string, liquid film-forming dressing that, upon application to intact skin, forms a protective film to help reduce friction during removal of tapes and films”. It contains alcohol, allows skin to “breathe”, and “removes easily using skin cleanser or soap and water”. (source:smith-nephew.com)
- Bard® Protective Barrier Film wipes prevents irritation by forming “a clear, breathable film… virtually impervious to adhesives, liquids and other potential irritants.” (source: www.woundcareshop.com)
- Cavilon™ No Sting Barrier Film (wipes) or Liquid Spray (manufactured by 3M) are a “liquid barrier film that protects intact or damaged skin from body fluids, friction, and adhesives. This fast-drying, alcohol-free liquid barrier film forms a breathable transparent coating on the skin. Cavilon™ is non-sticky and protects damaged or intact skin… is hypoallergenic, non-toxic and will not sting even when applied to damaged or denuded skin.” (source: diabetesexpress.ca)
- Nexcare™ No-Sting Liquid Bandage (by 3M™) “dries in 30 seconds and provides a skin shield that’s waterproof, so it lasts through several washings or in situations where you need to get wet, like swimming, (and) breathable… alcohol-free and contains no fragrance or preservatives”
More on Skin Prep:
Step 8. Use a Liquid Adhesive (to Increase Adhesion)
Expert- and User-approved
If you have problems with the infusion sets or sensors falling off early, before the life of the set/sensor is done, you may also want to try adding an adhesive layer on the skin as a tacky base, before applying adhesive products (sets and sensors). It’s important to note that such a product is not designed to reduce irritation per se (as are the products in Step 6, above), though some products do fulfill both purposes, keeping the set/sensor stuck on, and at the same time acting as an effective barrier between tape and skin. On the other hand, some users find that extra adhesives actually increase irritation. So give them a try, but be prepared to ditch it if the problems outweigh the benefits.
Also note that you should avoid blowing on the skin to dry an adhesive layer, as this may actually create problems with adhesion if the top layer dries while the liquid below does not. Some users have pointed out that in one device manufacturer’s online instructional videos, they advise against blowing on the area, but instead suggest letting it dry naturally.
Consider any one of the following adhesive products or trade names (in random order):
- Skin-Tac-H™ Adhesive Barrier Wipe (by Torbot Group), a latex-free, hypoallergenic, clear, non-rubber liquid adhesive which does not contain benzoin. Skin-Tac™ does contain alcohol, so it does double-duty to cleanse the skin as well as increasing adherence of the set or sensor.
- Osto Bond Skin Bond Adhesive is a waterproof “skin bond that contains latex to create a strong, sturdy and durable adhesion that is simultaneously gentle on the skin. Designed with Zinc Oxide to substantially reduce skin irritation (it) creates a gentle albeit sturdy bond between skin and appliance.” Comes in a can with a brush cap applicator. (source: vitalitymedical.com)
- Anti-Perspirant applied to the skin is useful when the adhesion problem involves excessive perspiration: Any antiperspirant – not deodorant – that you can get from your local drugstore, OR a clinical-strength Anti-Perspirant, such as Hypercare 20% Aluminum Chloride antiperspirant
- Mastisol® liquid adhesive, which is a “clear, non-irritating, and non-water-soluble liquid adhesive that secures the most difficult dressings for an extended period of time. Mastisol® is 7 to 10 times stickier than Compound Tincture of Benzoin” (source: diabetesexpress.ca). Mastisol seals out dirt and bacteria, reducing the “risk of infection, as well as reducing unscheduled set changes or dislodged sets.”
- Costume glue, such as Pros-Aide®, which is used to affix theatrical prosthetics such as moustaches, noses, warts and wounds. Pros-Aide® is “extremely resistant to water, sweat and other moisture… Non-toxic, latex free, water-based bond that is safe on skin… preferred adhesive in the medical, television and motion picture industries.” (source: amazon.ca) You can get costume glue anywhere you would buy Halloween costumes, or Theatre makeup. In Calgary, we have bought it at Don’s Hobby, a local costume shop.
More on Skin Prep:
Step 9. Add a Barrier Tape
Expert- and User-approved
The use of a physical barrier of tape, in addition to or instead of a barrier wipe, may also reduce irritation at the site of an infusion set or sensor. Whether or not this is a useful step depends on how well a given product fits the problem you are trying to solve. For example, to reduce an allergic reaction, our family found that using a thin or water-permeable tape (IV3000 or Hypafix, respectively) did not reduce the reaction at all. However, for minor irritations, a tape barrier may be just enough to solve your set/sensor issue. Also, any of the following may be used on top of the sensor or infusion set, to keep it securely in place (see Step 11, below).
Consider any one of the following adhesive tape trade names (in random order):
- Tegaderm™, IV300™, and OPSITE™ FlexiFix™ are thin, transparent film dressings available in a variety of formats, from pre-cut patches in a variety of sizes, to tape rolls. For example, OPSITE™ FlexiFix™ is available as a 10 metre roll of 10cm-wide tape, an economical alternative to pre-cut patches.
Tips from the Trenches
OPSITE™ FlexiFix™ is what we use. Since it comes in a roll, we can just cut a piece off of the roll in the right length for the job at hand. 10 cm wide is perfect to keep numbing cream against the skin, or to keep an infusion set or sensor in place. It even came in handy for non-diabetes tasks: when my daughter scraped her knee falling off her bike, we cut a longer length to keep a non-stick pad over the wound until it healed. ~Michelle
- IV3000™ is waterproof, permeable to water vapour from underneath the dressing, and uses a “low allergy adhesive” (source: diabetesexpress.ca)
- Bioclusive™ Transparent Film Dressing is a self-adhesive dressing consisting of a transparent semi-permeable polyurethane film coated with an acrylic adhesive. (source: woundsource.com)
- KT Tape® Kinesiology Tape/ KT tape spray. Kinesiology Tape is the colourful tape that athletes use to support a muscle during training or competition. It can be useful either under or over an insulin pump infusion set, or CGM/Flash sensor.
- GrifGrip Patches were created to be “strong, secure, gentle, breathable, cost effective and most of all, let people move” by d-parents in the USA. They have a wide range of adhesive products for just about any make or model of d-tech, in a variety of colourful and fun patterns (including the option to design your own custom patches). www.grifgrips.com
- RockaDex adhesives are fun, colourful tapes and patches made specifically to fit with various insulin pump sets and glucose sensors. They come in a variety of shapes, colours and patterns, or on a tape roll. The company was started by a d-mom in Australia; their products are available in other countries as well.rockadex.com.au
- 3M Medipore™ H-Soft Cloth Surgical Tape, or similarly, Hypafix® Dressing Retention Tape are self-adhesive, breathable (allows moisture to evaporate), water-resistant (not water-proof), latex-free, easy to remove, “non-woven fabric sheets for secure and rapid fixation. (Hypafix®) is made from white polyester material and coated with hypoallergenic adhesive.”
- Hydrocolloid Adhesive Pads are a thick, rubbery patches which are “super tough”, “100% waterproof and sweat proof”, and are typically used to “seal wounds to promote faster healing.” They are much thicker than the thin, transparent dressings mentioned above, and because of this, as well as their waterproof construction, they may succeed where other water-permeable barrier tapes fail, in providing protection from major skin reactions.
Tradenames for Hydrocolloid Adhesive Pads include: Band-aid® Advanced Healing Pads, Band-Aid® HydroSeal™ patches (previously marketed in the USA as “Tough Pads”); Compeed®; DuoDERM®. Some users who did not find enough protection with the above Band-aid® products have found success with DuoDERM® – one even called it the “gold standard,” so it may be worth a try if you have not had success with other products.
There is some debate about whether or not you should cut a hole in the hydrocolloid pad before inserting the sensor or infusion set. Some users say they punch right through it with no problem, others say they have to cut a hole or risk ruining the sensor or set. Some users report that if they don’t cut a hole in the pad, the sensor fails within a few days (perhaps the sensor filament isn’t seated deeply enough into the fat layer due to the extra thickness?) Some users say that if they cut a hole, they still get a reaction where the irritant gets past the pad to the skin; others say that they still get adequate protection even when there’s a hole in the pad. As with most things related to diabetes, individual results will vary, you may have to experiment to see what works for you / for your child.
If you decide to cut a hole in the hydrocolloid patch, you can do so with a crafting hole punch, or by folding the pad lightly in half and then in half again the other direction, then cutting off a tiny bit of the inner corner with a pair of clean, sharp scissors, leaving a small hole in the dead centre of the patch.
Step 10. Remove the Factory-installed Adhesive?
User-approved
Before they insert the infusion set or sensor as it comes assembled from the manufacturer, some users have found success with removing the factory-installed adhesive backing (as well as any residue), and then using an alternate (non-irritating) adhesive in its place (such as double-sided body/lingerie tape, or a liquid adhesive – see Step 8, above), with an adhesive patch over top of it all to keep it in place (see Step 12, below). As many users have commented, this may not be the first approach to try, and it does void any warranty on the sensor, but for those who have not found success with other strategies, this “last ditch” effort may be the only thing that allows them to continue using their Flash or Continuous Glucose Monitor.
One user has even shared their process on YouTube: Libre Freestyle 14 Day Sensor Adhesive Removal in English by A C (May 2019). (Be sure to review the warnings provided in the video description!)
Tips from the Trenches
Some Libre users in some countries report as of September 2019 that newer sensors no longer cause a reaction as they did previously. There has been no official statement from Abbot on this topic, which means either there has been no change in formulation, or the company is trying to stay under the radar on this. Their position has always been that the incidence of skin reactions to this product is low. At this time, users in other countries continue to report the occurrence of adverse events when they use Flash.
Step 11. Insert the Sensor or Infusion Set
Having applied one or more of the previous steps, now is the time to insert the insulin pump infusion set, CGM sensor, or Libre sensor, according to manufacturer directions for that device.
Some users have found that the skin on some parts of their body is more sensitive than others, and that eliminating reactions is as easy as moving the insertion site to a new location, where the skin is tougher, more resistant to irritation.
More on Site Locations:
More on Inserting:
Step 12. Add an Overlay of Protective Tape
Expert- and User-approved
Most of the products listed in Step 9 (above – EXCEPT Hydrocolloid Adhesive Pads) may be used on top of the sensor or infusion set, to keep it securely in place.
For convenience, Smith&Nephew makes an IV 3000 patch (6cm x 7cm) for infusion sets with a hole pre-punched in the middle, for the plastic housing of the set or sensor to poke through. Why is this useful? Leaving a sensor uncovered may help reduce the occurrence of “signal loss”, in which the transmitter is unable to send the glucose reading to the receiver, leaving gaps in your glucose data. It can also be a pain to get the sticky residue from adhesive tapes off of the back of the re-useable CGM transmitter so that you can pop it into the next sensor housing – if the tape goes around the transmitter instead of on top of it, then there’s no sticky residue on the transmitter itself, saving you a step.
If you want to avoid the expense of pre-punched tape patches, you can cut a hole in a patch yourself by folding the pad lightly in half and then in half again the other direction, then cutting a rounded or square hole from the inner corner with a pair of clean, sharp scissors, leaving a gap in the centre of the patch that approximately matches the particular shape of that brand of infusion set or sensor housing.
Step 13. Adhesive Remover to Take Off the Set/Sensor
Expert- and User-approved
When it's time to change the set or sensor, if the products have done their job well (or even a little TOO well!), then pulling off a well-adhered set or sensor may damage the skin under it. To prevent this, you may want to use an adhesive remover to take the set or sensor off at the end of its recommended usage life (2-3 days for infusion sets, 7 or 14 days for CGM sensors, depending on manufacturer recommendations).
Consider any one of the following adhesive removers (in random order), when it’s time for a set change:
- Mineral oil or baby oil effectively removes adhesive residue (those black, sticky lines that stick around after the set/sensor is gone, usually where the edge of the tape sat). (User-approved)
- Remove™ Adhesive Removal Wipes (from Smith&Nephew), for the removal of adhesive devices (and) adhesive residue from skin. Remove “softens adhesive on tapes, films and appliances thereby minimizing trauma caused by adhesive removal”. (source: diabetesexpress.ca) Contains Aloe to condition the skin. (Expert-approved)
- TacAway® Adhesive Remover Wipes “provide one-step adhesive removal. Effectively removes even the most stubborn adhesive residue, leaving the skin clean and dry. No Greasy Residue!” (source: amazon.ca) TacAway is available as a bottle of liquid and in individual travel-friendly wipes. (Expert-approved)
- Aloe moisturizes and conditions skin, as well as promoting healing. It gently cleans hydrocolloid, acrylic and rubber-based adhesive residues from the skin. (User-approved)
- Goo Gone® is useful for getting adhesives and residue off of plastic products such as transmitters. For skin, it may be wise to use one of the gentler products designed specifically for use on skin, listed above. (User-approved)
More on Removing Sets & Sensors:
Step 14. Treat the Affected Skin (if needed)
Expert-approved
Despite your best attempts to reduce or eliminate inflammation and irritation, sometimes tender, itchy, red skin persists after you have removed an infusion set or sensor. For the best chance at successful healing, consider these first aid tips to avoid infection, promote healing, and reduce scarring:
- If the skin damage is significant, you may want see a doctor for advice and for prescription medications.
- Post-Inflammatory Steroid Cream. Hydrocortisone-Valerate Cream, such as HydroVal, is an anti-inflammatory (reduces inflammation, redness, swelling) and antipruritic (reduces itching) cream which is available in Canada by prescription only, so you will need to see your doctor to find out if this is an appropriate treatment for your individual situation. It has worked great for our family! (Expert-approved)
- Clean the wound by running cool water over the area, or for minor wounds, using an antiseptic wash such as Band-Aid Hurt-Free® (a liquid containing lidocaine hydrochloride which “relieves pain, cleanses wounds.”). Let it dry completely before applying any other products. (User-approved)
Tips from the Trenches
When our son’s skin blistered and broke because of a sensor, the damage was significant. We could only use water to clean the wound and it hurt (even air hurt!). An antiseptic wash was out of the question in this case, although we’ve used it effectively for other minor irritations. ~Michelle
- If the area is still itchy, you could apply an anti-itch spray or cream (such as Benadryl spray). (User-approved)
To manage pain and speed healing you could try (User-approved): - Aloe Vera extract
- Polysporin®Heal-Fast® Formula (a medicated cream which “prevents Infection, minimizes scarring, speeds healing”). The cream contains lidocaine hydrochloride for pain and 2 antibiotics (Polymyxin B Sulfate and Gramicidin) to prevent or treat an infection.
- Moist wound healing results in faster healing and less scarring than if the wound dries out and forms a scab first. You could cover the wound with a band-aid, a hydrocolloid patch, or a non-stick pad held in place with transparent film (such as Opsite™ Flexifix™). (User-approved)
Step 15. Share Your Experience
Some of the most valuable things that our family has learned about managing diabetes, we have learned from others in the diabetes community; skin reactions and keeping sets stuck on are no exception. If your child has a serious adverse reaction to an infusion set or sensor, consider these follow-up steps.
- Share your experience by reporting it to the company. They need to know about the problems that may be associated with their product. Also, they may be able to provide suggestions to avoid the problem in the future.
- Report your experience to Health Canada. Intervention with regards to a problematic health or medical product will only happen if Health Canada is made aware of these adverse reactions that the population is experiencing.
- Connect online with other diabetes tech users who have experienced obstacles in the use of these devices, for example on: Facebook “Dexcom and Libre Rash” group
Tips from the Trenches
What do YOU do to manage skin irritation with Flash and CGM sensors?
I recommend a skin prep wipe, then hypafix under the Libre sensor. ~Diabetes nurse/CDE
“I have found success with spraying Benadryl spray on the site and letting it dry completely then using band aid hydro seal (hydrocolloid) XL. I do cut a hole because otherwise it fails. I warm the hydro seal on my belly by holding it there for several minutes. Then I adhere it to the sensor adhesive to easily line up the small holes.” ~CGM user
I use two alcohol wipes first, let it dry, then apply 3 sprays of Trio Elisse, let each spray dry before applying the next layer, then a couple of sprays of the Piriton Nasal Spray, let it dry completely & then apply the sensor. It did come away a little bit on one side at about day 10 so I used an adhesive patch from Type 1 Badass from eBay. It stayed stuck & was accurate the whole time. ~CGM/Flash User
Spray it first with Benadryl spray, then a barrier wipe like Cavilon or Skin Prep, then a layer of OPSITE, then punch the sensor right through the OPSITE. ~Diabetes Specialist/CDE
Do you have a process that works for your family to keep sets/sensors on, and to avoid skin reactions???? We would love to hear from you:
SHARE THIS ARTICLE